SAN DIEGO – Sometimes, scientific breakthroughs occur when researchers aren’t exactly looking for them. While attempting to better understand the function of a protein in connective tissue cells, UC San Diego School of Medicine scientists found a way to transform multiple types of cells into neurons. This discovery has led to the development of a treatment that eliminates symptoms of Parkinson’s disease in mice.
The protein researchers were studying, called PTB, is known for its general role in activating or deactivating genes within a cell. In an attempt to better understand how PTB contributes to cell function, researchers silenced the PTB gene using a technique called siRNA in a type of connective tissue cell, known as a fibroblast. The researchers grew the fibroblasts in petri dishes, silenced PTB, and waited a couple of weeks to check on the fibroblasts and observe any changes.
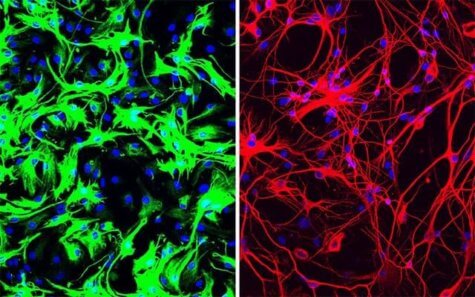
When the researchers checked the fibroblasts, they were shocked. They found that very few fibroblasts remained in the dishes. Instead, the dishes contained mostly neurons. Unintentionally, they had discovered a way to turn fibroblasts into neurons.
In subsequent experiments, the researchers found that they could also turn other cells into neurons. When they silenced PTB in a type of non-neuronal brain cell known as an astrocyte, they were also able to generate neurons.
“Researchers around the world have tried many ways to generate neurons in the lab, using stem cells and other means, so we can study them better, as well as to use them to replace lost neurons in neurodegenerative diseases,” says lead author of the study, Xiang-Dong Fu, in a release. “The fact that we could produce so many neurons in such a relatively easy way came as a big surprise.”
Fu is a Distinguished Professor in the Department of Cellular and Molecular Medicine at UC San Diego School of Medicine.
Scientists ‘stunned’ after Parkinson’s disease test
Once researchers realized that they could easily create neurons from other types of cells, they decided to see if the method could be used to treat neurodegenerative diseases, such as Parkinson’s disease. In Parkinson’s, dopamine cells in the brain die. Thus, to assess their method, the researchers used a chemical that poisons dopamine neurons and creates symptoms of Parkinson’s disease in mice.
After using the chemical to kill dopamine neurons in the mice, researchers silenced PTB. They found that 30% of astrocytes turned into neurons. Moreover, these newly generated neurons seemed to grow normally and even began to send connections to other parts of the brain, like normal neurons.
When the researchers looked at mouse behavior, they also found that silencing PTB completely restored movement function. Moreover, even though the PTB-silencing treatment was only administered once, the mice did not show any symptoms of Parkinson’s disease for the remainder of their lifetime.
“I was stunned at what I saw,” said study co-author Dr. William Mobley, Distinguished Professor of Neurosciences at UCSD’s School of Medicine. “This whole new strategy for treating neurodegeneration gives hope that it may be possible to help even those with advanced disease.”
Not quite ready for humans
While the treatment is promising for the treatment of neurodegenerative diseases in humans, it still needs to go through more rigorous testing before being ready for human trials. In the next steps, the researchers plan to test the method with other mouse models of Parkinson’s disease. These models involve genetic changes rather than chemical destruction of dopamine neurons.
The researchers have also patented their treatment in hopes of moving it forward to testing in humans.
“It’s my dream to see this through to clinical trials, to test this approach as a treatment for Parkinson’s disease, but also many other diseases where neurons are lost, such as Alzheimer’s and Huntington’s diseases and stroke,” Fu says. “And dreaming even bigger — what if we could target PTB to correct defects in other parts of the brain, to treat things like inherited brain defects?”
“I intend to spend the rest of my career answering these questions,” he says.
The study is published in Nature.
Like studies? Follow us on Facebook!

If it truly shows promise withhold the therapy from humans especially with those who have little
to lose. Too much red tape, too much safety first, If we did this with “the Vaccine” we would still be in the pandemic. Instead we have millions of mice test models in the form of humans mandated to receive the shot without any knowledge of the long term consequences of the therapy. I for one would gladly take a chance for improved quality of life over “safety” even if it meant that there was a chance of shortening my life by a few years, I believe it is about the quality of life not the quantity of life. A long term progressive disease is no fun living for the patient or loved ones. Show me the way to a cure not masking of symptoms.
I echo your comments Jim. When it comes to breakthroughs that can actually save lives, too much red tape. But well done to the researchers. Hoping this can be fast tracked.