
TEL AVIV, Israel — A groundbreaking new procedure has found a way to turn belly fat into a material which can repair spinal cord damage that leaves patients paralyzed. Researchers from Tel Aviv University say implanting the genetically engineered tissue sample into the spines of mice allowed the animals to walk again.
This tissue comes from the actual patient, making every sample a personalized implant for the spinal cord. In experiments, the “world first” technique restored mobility in nearly all mice. The tissue mimics development of the spinal cord in human embryos. Study authors call their results “highly encouraging.” Clinical trials are already in the planning phase.
Professor Tal Dvir notes that the mice underwent a rapid rehabilitation process, ending with the animals walking quite well after their procedures. It’s the first time an implanted engineered human tissue has led to a successful recovery in an animal dealing with long-term chronic paralysis.
The implants come from the patient’s own body
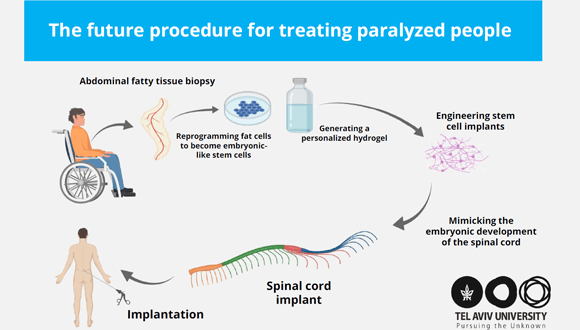
The fully personalized implant consists of the patient’s own materials and cells. That means there is no need for immunosuppressant drugs, which can endanger the patient’s health. In the study, scientists extracted fatty tissue from the patients’ stomachs and separated cells from acellular material.
The researchers then manipulated the samples into pluripotent stem cells that can turn into any kind of cell — from neurons to cardiac cells to spinal cord cells. They also transformed the acellular material into a personalized hydrogel that supports cells and allows them to form a functioning tissue.
Combining that material with the newly formed stem cells created the spinal cord implant. Studies using animal and human blood have previously shown the patient-specific biomaterials do not induce an immune response.
“Our technology is based on taking a small biopsy of belly fat tissue from the patient,” explains Prof. Dvir, the research leader, in a university release. “This tissue, like all tissues in our body, consists of cells together with an extracellular matrix comprising substances like collagens and sugars. After separating the cells from the extracellular matrix we used genetic engineering to reprogram the cells, reverting them to a state that resembles embryonic stem cells – namely cells capable of becoming any type of cell in the body.”
The goal is to cure ‘every paralyzed person’
In this experiment, scientists used the 3D implants to form neuronal networks containing motor neurons. They hope paralyzed individuals will be receiving the engineered devices within a few years, enabling them to stand up and walk again.
In the United States, there are about 296,000 Americans currently living with a spinal cord injury and doctors diagnose about 17,900 new SCI cases each year. There is still no effective treatment for their condition.
“Our goal is to produce personalized spinal cord implants for every paralyzed person, enabling regeneration of the damaged tissue with no risk of rejection,” Prof. Dvir says.
The implants, described in the journal Advanced Science, were transplanted into two groups of mice. Afterwards, 100 percent of “acute” recently paralyzed animals regained their ability to walk. There was also an 80 percent success rate among “chronic” patients with long-term paralysis — the medical equivalent of a year in human terms.
Three years ago, Prof. Dvir teamed up with industry partners to establish Matricelf (matricelf.com) in 2019. The company applies his approach in the aims of making spinal cord implants commercially available for persons suffering from paralysis.
“We hope to reach the stage of clinical trials in humans within the next few years, and ultimately get these patients back on their feet. The company’s preclinical program has already been discussed with the FDA. Since we are proposing an advanced technology in regenerative medicine, and since at present there is no alternative for paralyzed patients, we have good reason to expect relatively rapid approval of our technology,” Prof. Dvir concludes.
South West News Service writer Mark Waghorn contributed to this report.
