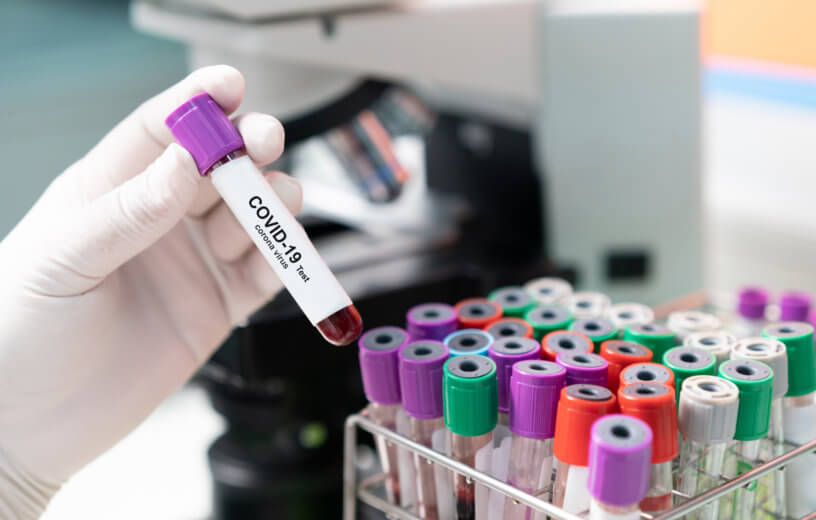
LA JOLLA, Calif. — To be immune, or not to be immune: that is the question. As the number of COVID-19 cases continue to rise, it remains unclear whether patients can become immune to SARS-CoV-2, the novel coronavirus that causes this disease. Scientists with the La Jolla Institute for Immunology now believe they’re closer to a firm answer. A recent study of theirs shows that individuals who recovered from COVID-19 did indeed mount a robust immune response against the virus.
Of course, the answer to this question holds important implications for individuals who were previously infected with the virus, as well as for the success of vaccine development. The study, published in Cell, is the first to look specifically at the human T cell response to COVID-19.
How T Cells Affect Immunity
While much of the vaccine effort for COVID-19 has focused on developing antibodies against the virus, it is clear that T cells also represent an important component of immunity. There are two main types of T cells in humans: CD8 “killer” T cells which help eliminate virus-infected cells; and CD4 “helper” T cells which bolster the ability of B cells to produce atibodies. Both types of T cells are induced in antiviral responses to other coronaviruses, including the closely related SARS virus. However the magnitude and composition of these responses have yet to be characterized in SARS-CoV-2.
In addition, there is an urgency to understand whether T cell responses that are induced in COVID-19 correlate with protective immunity, so that more effective vaccines can be designed and tested.
Examining T Cells From COVID-19 Patients
In previous research, the authors used bioinformatics tools to predict which parts of SARS-CoV-2 might be capable of activating human T cells. For this latest study, the group tested whether T cells isolated from adults who had recovered from COVID-19 without major complications could recognize and respond to these predicted protein fragments. They showed that 100% of the patients produced a strong CD4 T cell response, and almost all (70%) of them had a virus-specific CD8 T cell response.

All patients were also positive for antibodies against SARS-CoV-2.
“If we had seen only marginal immune responses, we would have been concerned,” says Alessandro Sette, a professor in the Center for Infectious Disease and Vaccine Research, in a statement. “But what we see is a very robust T cell response against the spike protein, which is the target of most ongoing COVID-19 efforts, as well as other viral proteins. These findings are really good news for vaccine development.”
The authors mention that they specifically wanted to look at patients who did not require hospitalization so they could visualize what a normal immune response to the virus might look like. These results provide an important baseline against which to compare the immune responses of more severe patients. They also will help determine whether a candidate vaccine can produce an immune response that would approximate what you would see in natural infection.
“Our data show that the virus induces what you would expect from a typical, successful antiviral response,” says Shane Crotty, one of the study’s co-authors.
Could Other Coronavirus Strains Impact Immune Response Against SARS-CoV-2?
The study also investigated whether infection with any of the previously circulating human coronaviruses could result in cross-reactive immunity against SARS-CoV-2. To this end, the team looked at virus-specific T cell responses in blood samples collected from healthy, unexposed donors. The samples were collected between 2015 and 2018, before SARS-CoV-2 is believed to have emerged.
All blood samples from unexposed donors in this study tested positive for antibodies against OC43 and NL63 — two of the four human coronaviruses known to be causes of seasonal “common cold.” Many of these samples also showed significant T cell responses to SARS-CoV-2, despite having never been exposed.
The presence of these cross-reactive T cell responses raises the possibility that some level of pre-existing immunity to SARS-CoV-2 might exist in the population. However more research must be done before that can be confirmed.
Positive Outlook For Vaccine Development
Overall, the evidence gathered by this study supports the presence of a strong immune response in patients who have recovered from COVID-19, which is good news for vaccine developers. In addition, knowledge about SARS-CoV-2 immunity has implications for future pandemic control measures which can differ dramatically based on whether infection creates substantial immunity.
As Crotty notes, “All efforts to predict the best vaccine candidates and fine-tune pandemic control measures hinge on understanding the immune response to the virus.”
Like studies? Follow us on Facebook!