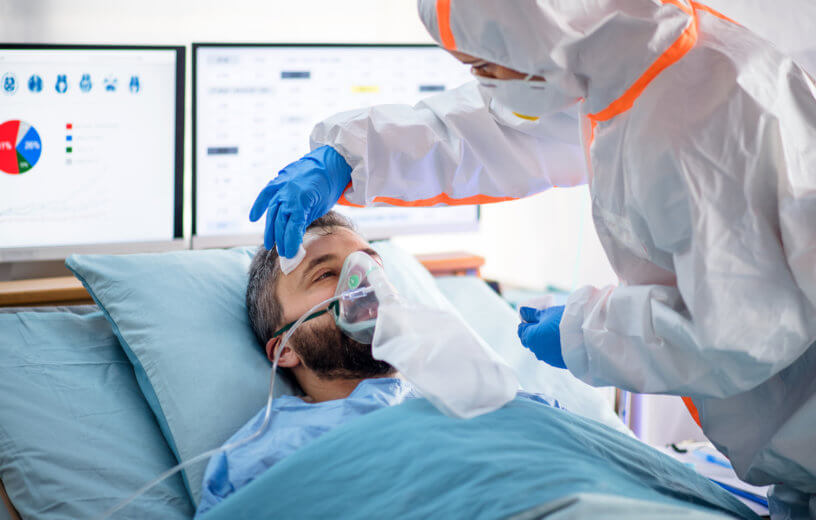
ANN ARBOR, Mich. — It’s safe to say most people can agree hospitals are places where people go to feel better. During the coronavirus pandemic however, a new study reveals about half of all COVID patients are actually leaving hospitals in worse shape than when they entered. In another case of COVID “long-hauler” side-effects, a team from Michigan Medicine says around 45 percent of patients who survive the virus exit the hospital with significantly less physical function.
“Rehabilitation needs were really, really common for these patients,” says pediatric physiatrist Alecia K. Daunter, M.D., in a university release. “They survived, but these people left the hospital in worse physical condition than they started. If they needed outpatient therapy or are now walking with a cane, something happened that impacted their discharge plan.”
Researchers reviewed the health data of almost 300 adults hospitalized with COVID-19 between March and April 2020. This information included discharge data, each patient’s therapy needs, and whether they needed special medical equipment or services after leaving the hospital.
The findings reveal doctors prescribed additional therapy for a staggering 80 percent of COVID-19 patients. Concerningly, nearly one in five patients lost so much of their physical ability they could no longer live independently after leaving the hospital.
“These patients may have needed to move to a subacute facility, or they might have needed to move in with a family member, but they were not able to go home,” Daunter adds. “This has a massive impact on patients and their families – emotionally and physically.”
The problem may be worse than the study shows
Researchers note their data comes from the pandemic’s first two months, at the very start of the first wave. At that time, not only did doctors not have a full picture of COVID’s effects, study authors say hospitals had to prioritize treating and releasing patients in order to free up bed space. With this in mind, Dr. Daunter believes the study is actually underreporting the number of COVID survivors who are losing their ability to live a normal life.
“Physicians and others in the health care system were working appropriately to discharge patients,” the lead author says. “They needed to keep patients safe while maximizing available beds and minimizing exposure to staff. I think that contributed to many people not being assessed by a therapist or PM&R physician. So, the things we do to in the hospital to maximize functioning, like mobility interventions and assessing activities of daily living were, not happening as often.”
Moving from COVID treatment to COVID rehabilitation
Study authors note that COVID-19 can systematically damage several organs throughout the human body. This trauma can result in neurological and musculoskeletal impairments which lasts for months after the infection clears. Michigan Medicine has even opened two new clinics to specifically address the issues COVID long haulers are facing.
Michigan Medicine physiatrist Edward Claflin says, even as the death toll drops and vaccinations continue, more and more people are now living with debilitating side-effects of their infection.
“These results help to highlight the true impact of the COVID-19 disease on our patients,” Claflin says. “They fill in that gap in knowledge about how patients with COVID recover and what kind of rehabilitation needs they have.”
“These problems are frequent, and the stakes are pretty high if we miss them, or allow them to progress during hospitalization,” Daunter concludes. “Some of these people were working and many were living independently. To lose that level of function is meaningful. We want to make sure we’re addressing those needs, not just looking at the black and white, survival or death.”
The study appears in the journal PM&R.