NEW YORK – Biopsies are a great tool for cancer screenings but it can take days to know the results. Researchers from Columbia University propose an alternative tool that is expected to speed up the rate of diagnosis and potentially improve treatments. MediSCAPE is a high-speed 3D microscope that is capable of imaging tissue structures in real-time.
Biopsies require doctors to cut out a small piece of tissue which is then stained with dyes and viewed by a pathologist using a simple microscope. But with MediSCAPE, imaging takes place inside the body and would also remove the need to remove tissues and wait for lab testing to be completed.
“Such a technology could give a doctor real-time feedback about what type of tissue they are looking at without the long wait,” says senior author Elizabeth Hillman, a professor of biomedical engineering and radiology at Columbia, in a statement. “This instant answer would let them make informed decisions about how best to cut out a tumor and ensure there is none left behind.”
According to the research team, another benefit to using MediSCAPE is avoiding the possibility of cutting out an important tissue section in the brain, spinal cord, nerves, eye, and face areas that could cause long-term damage to the person. “Because we can image the living tissue, without cutting it out, we hope that MediSCAPE will make those decisions a thing of the past,” Dr. Hillman says.
Dr. Hillman and her team have been creating and optimizing microscopes that could capture fast 3D images of living samples including worms, fish, and flies to examine brain activity when they move. They applied their microscopic technology to tissues from multiple body areas.
“One of the first tissues we looked at was fresh mouse kidney, and we were stunned to see gorgeous structures that looked a lot like what you get with standard histology,” says Kripa Patel, PhD, lead author of the study. “Most importantly, we didn’t add any dyes to the mouse — everything we saw was natural fluorescence in the tissue that is usually too weak to see. Our microscope is so efficient that we could see these weak signals well, even though we were also imaging whole 3D volumes at speeds fast enough to rove around in real time, scanning different areas of the tissue as if we were holding a flashlight.”
Further exploration led to a large data set that could create a 3D representation of tissue, comparable to a pathologist examining tissue samples in a box of slides.
“We found many examples where we would not have been able to identify a structure from a 2D section on a histology slide, but in 3D we could clearly see its shape. In renal pathology in particular, where we routinely work with very limited amounts of tissue, the more information we can derive from the sample, the better for delivering more effective patient care,” says Dr. Shana Coley, a renal pathologist at Columbia University Medical Center.
The team successfully used MediSCAPE in various scenarios from identifying pancreatic cancer in a mouse to observing signs of kidney disease from fresh samples of human kidneys. They also found that imaging tissues while still alive in the body could give them more information than resected and dead tissue samples. For instance, MediSCAPE detected blood flow through tissues and the cellular-level effects of ischemia and reperfusion.
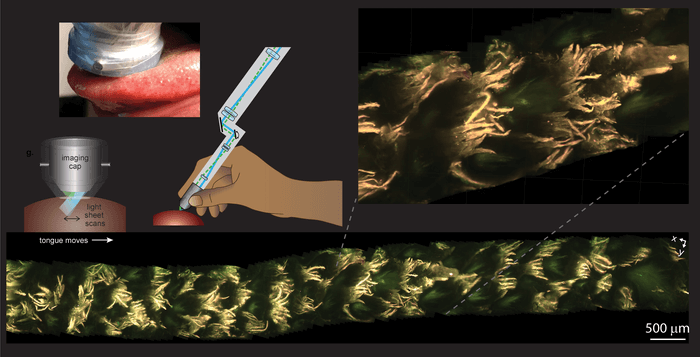
Although to use the 3D microscope to examine tissues, it has to fit into an operating room. Fortunately, the team developed a smaller version of the system along with a sterile imaging cap. In the first test on a living human, MediSCAPE was successful in collecting tissues in and around the mouth.
The study is published in the journal Nature Biomedical Engineering.

Wondering if this type of 3D ‘biopsy’ scan will allow for the scanning of bone tissue as well, allowing patients of Leukemia and other bone/blood-related cancers to avoid the traditional excruciating bone marrow biopsy procedure. If so, this is definitely an AMAZING breakthrough.