HOUSTON, Texas — Can what’s going on in your gut really change your blood pressure for better or worse? Researchers from Baylor College of Medicine say not only can the gut microbiome influence heart health, how people eat can determine whether those organisms help or hurt blood pressure levels. When it comes to diet, their study finds intermittent fasting can actually reshape the gut health of people with hypertension.
“Previous studies from our lab have shown that the composition of the gut microbiota in animal models of hypertension, such as the SHRSP (spontaneously hypertensive stroke-prone) rat model, is different from that in animals with normal blood pressure,” says Dr. David Durgan, assistant professor of anesthesiology at Baylor, in a university release.
Durgan adds there is growing evidence that disruptions in a patient’s gut microbiota (gut dysbiosis) can negatively impact blood pressure. Furthering this point, studies have even discovered that exposure to these disrupted microbes can affect healthy patients too. Transplanting dysbiotic gut microbiota from hypertensive mice to healthy ones results in the recipients developing high blood pressure as well.
“This result told us that gut dysbiosis is not just a consequence of hypertension, but is actually involved in causing it,” Durgan explains. “This ground work led to the current study in which we proposed to answer two questions. First, can we manipulate the dysbiotic microbiota to either prevent or relieve hypertension? Second, how are the gut microbes influencing the animal’s blood pressure?”
The right dieting habits can reshape an unhealthy gut
To answer their questions, researchers examined two groups containing both normal lab rats and SHRSP rats. One group allowed both hypertensive and normal rats to enjoy unrestricted food availability, serving as a control group. With the other group however, researchers only fed the rats every other day.
After nine weeks, study authors discovered, as expected, that SHRSP rats in the control group had higher blood pressure readings than normal rats. Those in the intermittent fasting group however, displayed significantly lower blood pressure in comparison to those not on a diet.
“Next, we investigated whether the microbiota was involved in the reduction of blood pressure we observed in the SHRSP rats that had fasted,” Durgan says.
Like the other studies, researchers transplanted microbiota from these rats into germ-free rats. These animals have no microbiota of their own which could throw off the results.
The results reveal germ-free rats receiving microbiota from SHRSP rats on normal diets developed higher blood pressure than those receiving microbiota from either the normal rats or the fasting group.
“It was particularly interesting to see that the germ-free rats that received microbiota from the fasting SHRSP rats had significantly lower the blood pressure than the rats that had received microbiota from SHRSP control rats,” Durgan notes. “These results demonstrated that the alterations to the microbiota induced by fasting were sufficient to mediate the blood pressure-lowering effect of intermittent fasting.”
The gut needs more acid to keep the body healthy
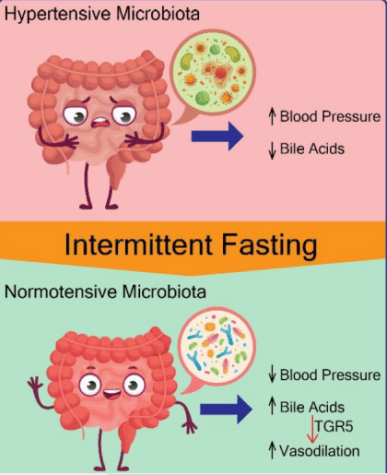
The findings left researchers with only one question, how does the gut microbiome actually lower blood pressure? The answer appears to come down to the amount of beneficial acid in a patient’s gut, with more being better.
“We applied whole genome shotgun sequence analysis of the microbiota as well as untargeted metabolomics analysis of plasma and gastrointestinal luminal content. Among the changes we observed, alterations in products of bile acid metabolism stood out as potential mediators of blood pressure regulation,” Durgan reports.
The team’s analysis finds SHRSP hypertensive animals eating normally have less bile acids circulating than rats with normal blood pressure. However, SHRSP animals in the intermittent fasting group had more bile acids in their systems.
“Supporting this finding, we found that supplementing animals with cholic acid, a primary bile acid, also significantly reduced blood pressure in the SHRSP model of hypertension,” the Baylor researcher adds.
“Taken together, the study shows for the first time that intermittent fasting can be beneficial in terms of reducing hypertension by reshaping the composition of gut microbiota in an animal model,” Durgan concludes. “Fasting schedules could one day help regulate the activity of gut microbial populations to naturally provide health benefits.”
The study appears in the journal Circulation Research.