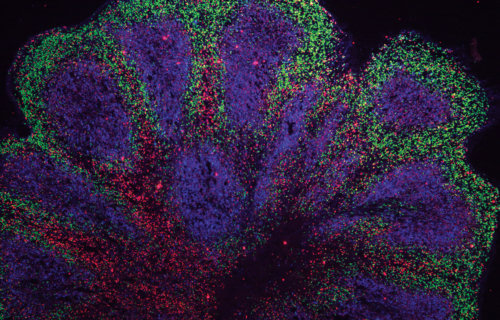
CAMBRIDGE, England — Around 55 million people currently suffer from dementia, and due to aging populations, cases worldwide are set to triple to 150 million by 2050. British scientists may have developed a breakthrough method for keeping that number down in the coming years. By creating miniature brains grown from the cells of dementia and motor neuron disease patients, researchers are opening the door for stronger treatments. In fact, scientists say one medication was found to destroy toxic proteins that gather in clump.
This fascinating trial also opens the door to personalized drugs based on an individuals’ own “mini-brain” developed from skin cells. The models were cultivated for almost a year, enabling analysis of dementia-related disorders over a long period. They were derived from patients with frontotemporal dementia (FTD) and amyotrophic lateral sclerosis (ALS), a more common form of motor neuron disease. Both conditions cause muscle weakness, as well as memory, behavior, and personality problems, and can affect people in their 30s and 40s. Famous physicist and cosmologist Stephen Hawking died in 2018 after being ravaged by ALS for more than 50 years.
“Neurodegenerative diseases are very complex disorders that can affect many different cell types and how these cells interact at different times as the diseases progress. To come close to capturing this complexity, we need models that are more long-lived and replicate the composition of those human brain cell populations in which disturbances typically occur, and this is what our approach offers,” says the study’s senior author, Dr. Andras Lakatos, in a statement. “Not only can we see what may happen early on in the disease — long before a patient might experience any symptoms — but we can also begin to see how the disturbances change over time in each cell,”
Mini-brains could allow doctors to effectively treat patients sooner
The mini-brains, or “organoids,” show what happens in the brain cells long before symptoms emerge and can screen potential therapies. One of the reasons drug trials have failed to date is that they are prescribed too late: once dementia or motor neuron disease has taken hold.
Brain tissue previously created in the lab has only lasted a short time, limiting the scope for experiments. The Cambridge team’s tissue survived for up to 340 days and harbored the most common genetic mutation in FTD and ALS. The 3-D cultures were cut into slices, ensuring they received the necessary fuel.
“When the cells are clustered in larger spheres, those cells at the core may not receive sufficient nutrition, which may explain why previous attempts to grow organoids long term from patients’ cells have been difficult,” first author Dr. Kornelia Szebenyi explains.
The structures demonstrated changes occurring at a very early stage, including stress and damage to DNA that harmed proteins. Brain and nerve cells — called astroglia — were affected. They orchestrate muscle movements and mental abilities.
“Although these initial disturbances were subtle, we were surprised at just how early changes occurred in our human model of ALS/FTD. This and other recent studies suggest the damage may begin to accrue as soon as we are born. We will need more research to understand if this is in fact the case, or whether this process is brought forward in organoids by the artificial conditions in the dish,” Dr. Lakatos says.
Could one medication already be in the works?
The researchers report that one particular medication combated the accumulation of rogue proteins seen in FTD and ALS. The medication reduced cell stress and the loss of nerve cells, blocking one of the causes of the diseases. Similar more suitable drugs approved for human use are now being tested in clinical trials for neurodegenerative diseases.
“By modeling some of the mechanisms that lead to DNA damage in nerve cells and showing how these can lead to various cell dysfunctions, we may also be able to identify further potential drug targets,” says co-senior author Dr. Gabriel Balmus, from the Dementia Research Institute at Cambridge.
Animal models often do not show the same brain alterations seen in humans. The mini-brains have an advantage over animal models in that they resemble parts of the human cerebral cortex, the brain’s outer surface which controls consciousness, thought, emotion, reasoning, language, and memory.
“We currently have no very effective options for treating ALS/FTD, and while there is much more work to be done following our discovery, it at least offers hope that it may in time be possible to prevent or to slow down the disease process. It may also be possible in the future to take skin cells from a patient, reprogram them to grow their ‘mini brain’ and test which unique combination of drugs best suits their disease,” adds Dr. Lakatos.
The study is published in the journal Nature Neuroscience.
South West News Service writer Mark Waghorn contributed to this report.