NEW YORK — We’re all waiting and hoping for something, anything that will effectively stop COVID-19 from taking more lives. With a vaccine seemingly out of reach for the foreseeable future, scientists and doctors all over the world are doing their best to find the most efficient treatment options. Now, researchers from Mount Sinai Hospital and School of Medicine say that blood thinners may be able to improve hospitalized coronavirus patients’ chances of survival considerably.
Their research concluded that the majority of COVID-19 patients treated with blood thinners saw improved outcomes, even those placed in ICUs. All in all, the study’s authors believe they’ve found a potentially major avenue of COVID-19 treatment for hospitalized patients.
“This research demonstrates anticoagulants taken orally, subcutaneously, or intravenously may play a major role in caring for COVID-19 patients, and these may prevent possible deadly events associated with coronavirus, including heart attack, stroke, and pulmonary embolism,” says senior corresponding author Valentin Fuster, MD, PhD, Director of Mount Sinai Heart and Physician-in-Chief of The Mount Sinai Hospital, in a release. “Using anticoagulants should be considered when patients get admitted to the ER and have tested positive for COVID-19 to possibly improve outcomes. However, each case should be evaluated an individualized basis to account for potential bleeding risk.”
It’s recently come to light that many COVID-19 patients are experiencing potentially life-threatening blood clots. So, the benefits of blood thinners are no doubt tied to that.
A total of 2,773 COVID-19 patient records were analyzed for this research. All of those patients had been treated within the Mount Sinai NYC Health System between March 14th and April 11th of this year. More specifically, survival rates for patients given blood thinners were compared to survival rates among those not treated with blood thinners. That being said, researchers were sure to account for other potentially influential health factors, such as age, ethnicity, and pre-existing health conditions, before evaluating the effects of blood thinners.
Among all analyzed patients, 786 (28%) had received a “full treatment dose” of blood thinners. The dosages doled out to patients were higher than the average amount given for blood clot prevention, and more in line with what what’s given to people already suffering from a full blown blood clot. In short, blood thinner treatments were associated with higher hospital survival outcomes, across both ICU and non-ICU scenarios.
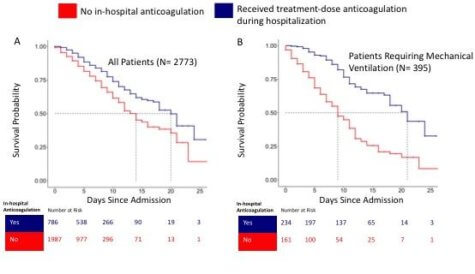
Patients who eventually passed away after being treated with blood thinners still survived longer on average (21 days) than patients who were not given blood thinners (14 days). Moreover, blood thinners appeared to be extra helpful for patients requiring ventilators. While 62.7% of ventilated patients who did not receive blood thinners passed away, only 29.1% of ventilated patients who were given blood thinners died.
“We are hopeful that this report of the association of anticoagulation therapy with improved survival will be confirmed in future investigations. The astute scientists at Mount Sinai continue to analyze our data on COVID-19 patients in order to contribute to worldwide efforts to find effective treatments,” comments David Reich, MD, President and Chief Operating Officer of The Mount Sinai Hospital.
Patients who received blood thinners also showed higher levels of bodily inflammation upon first being admitted to hospitals, so the study’s authors theorize that COVID-19 patients in critical condition can benefit from blood thinner treatments as early as possible.
“As a cardiologist who has been on service caring for COVID-19 patients for the last three weeks, I have observed an increased amount of blood clot cases among hospitalized patients, so it is critical to look at whether anticoagulants provide benefits for them,” says co-researcher Anu Lala, MD, Assistant Professor of Medicine (Cardiology) at the Icahn School of Medicine at Mount Sinai. “It’s important to note that further analysis and prospective studies are required to determine the effectiveness for widespread use of anticoagulants in hospitalized COVID-19 patients.”
The study is published in the Journal of the American College of Cardiology.
Like studies? Follow us on Facebook!
