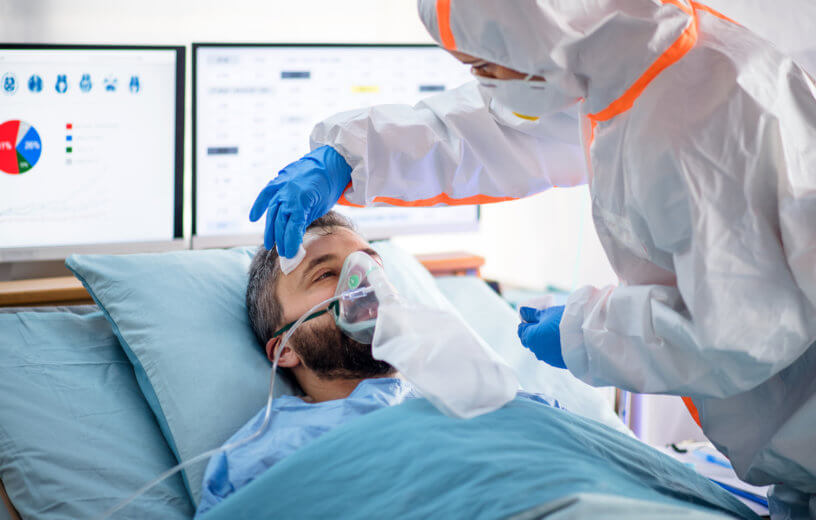
Doctors warn that the drug hydroxychloroquine may cause heart damage, Remdesivir may lead to low blood pressure or an irregular heartbeat.
CHARLOTTESVILLE, Va. — Ever since we learned of the novel coronavirus and the COVID-19 disease it causes people to focus on the effects the disease has on the respiratory system. Even the full name of the virus, Severe Acute Respiratory Syndrome Coronavirus 2, only mentions the respiratory side of the virus. New research from the University of Virginia shows that the disease also has a nasty cardiovascular side to it and can lead to complications including heart failure and blood clots that can lead to a heart attack or stroke.
A team of emergency-medicine doctors led by Dr. William Brody, reviewed research articles that mention keywords like “COVID-19,” “SARS-CoV-2,” “heart,” “cardiac,” or “cardiovascular.” The researchers examined a total of 45 articles for their study.
“In writing this article, we hope to increase emergency physicians’ knowledge and awareness of this new pathogen and its impact on the cardiovascular system,” says Brady, of UVA’s Department of Emergency Medicine, in a university release. “As we encounter more and more patients with COVID-19-related illness, we are increasing our understanding of its impact on the body in general and the cardiovascular system in particular. The rate of learning on this area is amazingly rapid. Information continues to change weekly, if not daily.”
The review shows that heart failure should be a major concern of emergency-medicine doctors. One of the studies found that 24% of COVID-19 patients were suffering from acute heart failure at the time they were diagnosed with COVID-19. The medical records of about half of the COVID-19 patients with heart failure show that they were not known to have high blood pressure or cardiovascular disease.
The authors note that this statistic does not mean that 24% of COVID-19 patients will eventually suffer heart failure. It’s unclear from this single study if the coronavirus causes heart failure or if it worsens undiagnosed heart failure.
The review also highlights the increased risk of heart attack and stroke caused by COVID-19 and other diseases that cause severe inflammation in the body. Severe inflammation can cause fatty plaque to build-up in the blood vessels and arteries, and they can eventually rupture and cause a heart attack or stroke. The papers reviewed show that influenza and several other viruses have been associated with plaque ruptures within the first week following diagnosis.
The authors also caution doctors to consider drug interactions when treating their COVID-19 patients. Some of the drugs being used to treat the disease can cause unwanted cardiovascular complications. For example, hydroxychloroquine can cause heart damage and worsen cardiomyopathy. It can also interact with drugs used to regulate heart rhythm. Similarly, an antiviral drug that the FDA has authorized for COVID-19 treatment, Remdesivir, can cause low blood pressure and cardiac arrhythmia.
“As we gain more experience with this new pathogen, we realize that its adverse impact extends beyond the respiratory system,” Brady says. “We will continue to learn more about COVID-19 and the most optimal means of managing its many presentations.”
The study is published in the American Journal of Emergency Medicine.