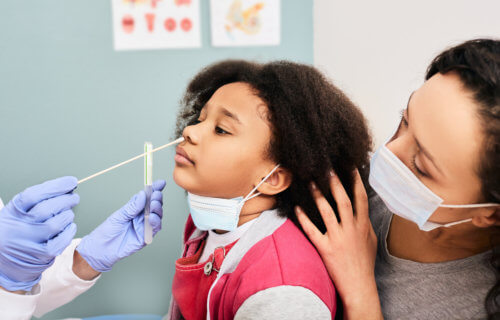
ITHACA, N.Y. — It’s anything but pleasant, but researchers from Cornell University say checking for COVID-19 using deep nostril swabs is the best way to test for SARS-CoV-2 infection.
More specifically, scientists found that nasopharyngeal swabs (where healthcare workers insert a swab far inside the nose) are more effective at detecting COVID than both saliva tests and swabs going just inside the nostril or under the tongue. Additionally, the study also notes detection rates were lower across the board among asymptomatic patients.
“The study addressed the very important issue of identifying a sample type that would allow reliable detection of the virus, without significantly compromising the sensitivity of detection,” says lead study author Dr. Diego Diel, associate professor in the Department of Population Medicine and Diagnostic Sciences and director of the virology laboratory at the Animal Health Diagnostic Center, in a university release.
To reach these conclusions, the team at Cornell gained access to samples from patients in Tompkins County, New York through a collaboration with Dr. Elizabeth Plocharczyk from the Cayuga Medical Center. In all, they used four distinct sample types: sublingual swabs (under the tongue), nasopharyngeal swabs, anterior nares swabs (front of the nostril), and saliva. They collected samples from symptomatic, asymptomatic, and post-symptomatic individuals.
A comparison of the different samples revealed that nasopharyngeal samples provided the best rate of detection (92-100%). This result isn’t all that shocking, considering the coronavirus replicates in the nasal turbinate, or the tissue structures in the uppermost nose area.
How do other testing methods compare?
Front of the nostril swabs and saliva tests displayed slightly lower detection rates (92-96%) among symptomatic patients – but detection rates were notably lower for these tests among asymptomatic patients (75-92%). Meanwhile, sublingual swabs proved the least accurate, with detection rates of only 40 to 60 percent among symptomatic patients and 25 to 42 percent among asymptomatic patients.
Across all considered test types, it’s easiest to identify COVID-19 when a patient is symptomatic (92-100% detection rate), but somewhat more difficult to detect in asymptomatic patients (75-96% detection rate). Once a patient fully recovers from COVID-19 symptoms (post-symptomatic), detection becomes much tougher.
Researchers also looked into infectivity, or the amount of infectious viral particles excreted in each of the sample types and from different patients. Sure enough, the most infectious samples came from symptomatic patients. Less than a third of the specimens from asymptomatic patients were infectious. Finally, study authors report they were unable to isolate any trace of the infectious virus from post-symptomatic patient samples.
“We were surprised at the relatively short period in which infectious virus was detected,” Prof. Diel adds. “The data is aligned with current CDC guidelines and their decision to decrease patient isolation periods from an initial 14-day period to 10 and ultimately to five.”
“This study served as the foundation for the Cornell COVID-19 surveillance program testing labs and confirmed the use of anterior nares specimens as the specimen of choice, given its reasonable sensitivity and ease of collection,” he concludes.
The findings appear in the journal Microbiology Spectrum.