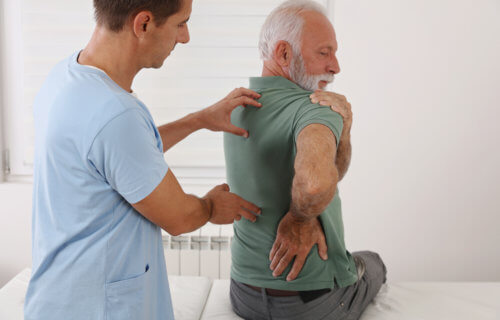
TAIPEI, Taiwan — Osteoarthritis, or degenerative joint disease, can be an extremely painful condition to have to manage as we age. Although patients typically feel its effects in the hands, back, knees, and hips, a new study reveals osteoarthritis may also lead to incurable damage in the brain. Researchers in Taiwan say older adults suffering from osteoarthritis are also at a much higher risk of developing Parkinson’s disease.
Parkinson’s is a progressive neurological disorder that causes nerve cells in the brain which control movement to break down and die due to oxidative stress. The disease leads to increasingly impaired movement, stiffness, and loss of balance. Patients also typically experience tremors in their hands and slurred speech which worsens with age.
For osteoarthritis patients, this particular type of arthritis develops when flexible tissue at the ends of the bones begins to wear down. As the protective tissue (cartilage) continues to wear down over time, the pain in the joints becomes even worse. Although scientists continue to work on treatments which slow the progression of both of these diseases, there is currently no cure for either one.
How does joint pain lead to neurological trouble?
Researchers examined the health records of 33,360 patients between 50 and 64 years-old from Taiwan’s Longitudinal Health Insurance Database. Each of these patients had osteoarthritis during the study period, between 2002 and 2005. Study authors compared this group to another batch of 33,360 patients in the same age range who did not have osteoarthritis.
Those results reveal that older adults with degenerative joint disease have a 41-percent higher risk of developing Parkinson’s disease. Researchers note this figure accounts for various health factors which could throw off the results.
Additionally, patients specifically dealing with knee or hip osteoarthritis appear to have even higher odds of developing Parkinson’s than other adults who have uncategorized osteoarthritis or joint pain in another area besides the knees or hips.
As for why these two conditions appear to have a connection, study authors say they aren’t sure, but both osteoarthritis and Parkinson’s disease involve inflammation. In fact, a previous study looking at the link between Parkinson’s and living near busy roadways discovered that toxic particles from those areas can travel through the bloodstream and into the brain. This causes inflammation and oxidative stress, possibly leading to neurological damage.
“Coexisting osteoarthritis and Parkinson’s disease can additively increase the risk of falling. Moreover, osteoarthritis-related mobility impairments may mask early motor symptoms of Parkinson’s disease,” says senior author Shin-Liang Pan, MD, PhD, of National Taiwan University in a media release. “Health professionals need to be alert to the potential link between these two diseases.”
The study appears in the journal Arthritis Care & Research.