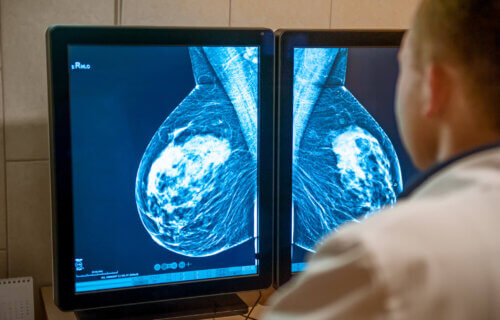
LONDON — Since the early 1990s, breast cancer cases have increased by about 21.9% in the U.S. In 2021, approximately 43,600 American women are expected to die of breast cancer. Regular mammograms are key to reducing the chances of dying from breast cancer, doctors say. In fact, a new study warns that women who skip just one breast scan before being diagnosed with cancer are “significantly” more likely to die.
General practitioners recommend breast cancer screenings every two years for women between the ages of 50-74. Mammograms help doctors catch cancers early when they are easier to treat and the chances of survival are high. However, researchers say despite their well-stabilized effectiveness, many women still take a rain check.
“Regular participation in all scheduled screens confers the greatest reduction in your risk of dying from breast cancer. The results add further evidence to support regular screening with mammography as a means for reducing breast cancer-related deaths,” says lead author Stephen Duffy, a professor of cancer screening at Queen Mary University of London, in a statement.
Data was analyzed from nearly 550,000 women in nine Swedish counties, with access to breast screenings between 1992 and 2016. They were divided into two groups based on whether they attended two of the most recent mammography screenings before being diagnosed with breast cancer. Women who attended both sessions were labeled “serial participants,” while those who missed them were categorized as “serial nonparticipants.”
Researchers found within 10 years of being diagnosed, 50% fewer serial participants had died. Likewise, women who attended only one of the two breast cancer screenings had 29% higher mortality than those who went to both.
“While we suspected that regular participation would confer a reduction greater than that with irregular participation, I think it is fair to say that we were slightly surprised by the size of the effect. The findings support the hypothesis that regular attendance reduces the opportunity for the cancer to grow before it is detected,” says Duffy.
To better understand the benefits of screenings, the researchers are continuing to analyze the data. In particular, they are focusing on interval cancers, which arise between X-ray sessions.
“We are planning further prognostic research into the mechanism of this effect. For example, we plan to investigate whether and to what extent regular attendance improves the prognosis of interval cancers as well as screen-detected cancers. Estimation of this by time since the last screen may have implications for policy on screening frequency,” adds Duffy.
The findings are published in the journal Radiology.
SWNS writer Tom Campbell contributed to this report.