WEST YORKSHIRE, England — Scientists may have made a major breakthrough in treating — and potentially defeating — cancerous brain tumors by injecting patients with a virus that actually stimulates the immune system.
Researchers at the University of Leeds conducted a study on nine patients battling fast-growing gliomas, which are aggressive tumors that are tough to treat and typically come with a grim outlook. The participants were scheduled to have the tumors removed surgically, but in the days prior to the procedure, they were injected with the naturally occurring “reovirus” through an IV drip.
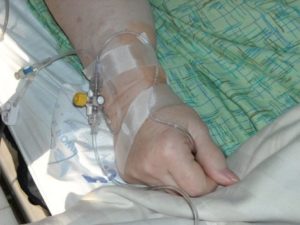
Reovirus has been shown to attack cancer cells without impacting healthier cells in the body.
Once in the bloodstream, the virus would have to pass through the protective membrane surrounding the brain known as the blood-brain barrier in order to take a toll on the tumors. If this could happen, they predicted the virus could replicate once inside the tumors and kill cancerous cells.
“Brain cancer is a devastating disease. For a long time, there have not been many new developments that we could offer patients but the research that is happening at the University Leeds and elsewhere is beginning to offer a new approach,” says Susan Short, Professor of Clinical Oncology at the school.
Still, the authors had cautious optimism in the virus passing through the barrier. They feared the attempt would fail and a more likely scenario would force them to have to inject the virus directly into the brain — a more delicate and dangerous procedure not suitable for all patients.
Incredibly, that predicament wouldn’t be necessary. After the tumors were removed from the patients, tests showed that the virus did in fact penetrate the barrier and reached the cancer in each patient. Moreover, the researchers discovered the virus stirred up the patients’ immune systems to battle back against the tumors, causing white blood cells to attack the cancerous ones.
“This is the first time it has been shown that a therapeutic virus is able to pass through the brain-blood barrier, and that opens up the possibility this type of immunotherapy could be used to treat more people with aggressive brain cancers,” says Dr Adel Samson, a medical oncologist and co-lead author of the study, in a university release.
Adds co-lead author Alan Melcher, a professor of translational immunotherapy at the Institute of Cancer Research in London: “Our immune systems aren’t very good at ‘seeing’ cancers — partly because cancer cells look like our body’s own cells, and partly because cancers are good at telling immune cells to turn a blind eye. But the immune system is very good at seeing viruses.”
Melcher says that once the tumors were infected with the reovirus, the cancer cells were then “visible” to the immune system. The team is now testing their results in a clinical trial where patients at the St. James Hospital in Leeds are being treated with the reovirus IV-drips in concert with other standard cancer treatments.
“Our hope is that the additional effect of the virus on enhancing the body’s immune response to the tumour will increase the amount of tumour cells that are killed by the standard treatment, radiotherapy and chemotherapy,” explains Short.
The study’s findings were published earlier this month in the journal Science Translational Medicine.
This was the etiology of how science wiped out the human race in the movie “I Am Legend”.
They didn’t wipe them out they turned into zombies. Huge difference.
Uh, yeah.
If you like zombies. I think I will stick with dogs, or at a pinch, those rare cats who act like dogs.
Makes me think of World War Z a little bit
FOR THE LOVE OF GOD, DON’T TELL McCAIN!!!!
My first thought too.
Hey, not nice. I’m not a big fan of him politically….however, when he was languishing in a POW camp I was drinking beer
on campus. I hope this cure is credible and he gets treatment. I hope he recovers……and then retires.
I respect his service, however, he’s been a RINO for a whole lot longer, sabotaging everything he can, especially what Trump has tried to do.
I’ll put this way: I’ve never wished death upon anyone but I look forward to reading some obituaries with great enthusiasm.
I agree with you on his RINO stuff. However we will have to agree to disagree on your death wish.
Again, I’ll put this way: I’ve never wished death upon anyone but I look forward to reading some obituaries with great enthusiasm.
I don’t wish him dead but won’t be sorry to see the old bastard go.
why all the accounts??
“Our hope is that the additional effect of the virus on enhancing the
body’s immune response to the tumour will increase the amount of tumour
cells that are killed by the standard treatment, radiotherapy and
chemotherapy,” explains Short.
Shouldn’t the hope be that when this treatment is perfected radiotherapy and chemotherapy will no longer be necessary or do the doctors want to continue billing for those as well?????
All those participating in the study would want the best chance of survival, no?
No because the Rockefellers wouldn’t get rich anymore from the chemo drugs that they peddle. I totally agree with you Harvey.
Yes, there is that job security thing in the cancer business even though I recently read they have laid off a large number of high level cancer researchers.
I love to read about these findings but have been doing so for so long that they have become meaningless. I’m surprised they didn’t end the story with the customary, “Well, the therapy has to go thru rigorous study and won’t be available for humans for at least 10 to 20 years.” Publish or perish.
They’ve also been trying this approach on melanoma for decades to no avail.
Don’t wait up.
I’m sure it will be available to the rich and famous first and everyone else will be secondary. Good post Harry.
Using pathogens to fight cancer by stimulating the immune system has a long history, including being excluded by the FDA. https://www.cancerresearch.org/blog/april-2015/what-ever-happened-to-coleys-toxins
the Reovirius has been fast tracked……see ONCYF if you wish to invest
Liberals are a far worse cancer than brain cancer.
ONCYF on the US otc exchange if you wish to invest
And as with most “breakthroughs”, once this news cycle runs out, we’ll hear about it again.
Goddamn it, can’t you at least wait until that treasonous, senile, Depends-soiling RINO McCain croaks? Please??
I think this will be the cure for many diseases that are being caused by actinomycetes bacteria I have systemic whipples disease and at first I thought maybe a bacteriophage would work now I’m thinking the reovirus could be a cure for whipple’s disease, cancer, diabetes, and alzheimers since research is showing that they’re all being caused by actinobacteria/actinomycetes. I wish I could get this to see if it would heal or cure me of my disease. I would love to be a guinea pig I’m getting sicker and worse from it anyway I have nothing to lose at this point. Antibiotics aren’t doing anything for me in regards to this. It always eventually becomes resistant to it over time doesn’t matter what it is. My email is [email protected] if anyone could help me please let me know thank you and God bless.
which means that our own body can fight off cancer. once that secret is found it shouldnt be that hard to start curing people. just need to make the tumors visible to the white cells, and then the white cells attack the cancer, so turning them from ghosts to being seen is all it takes.