ROCKVILLE, Md. — Unlike past coronavirus outbreaks, COVID-19 has kept the world locked down for over a year. Its unnerving infection rate, which has led to over 100 million cases worldwide, surpasses even the SARS epidemic of 2003. Now, a new study has discovered what makes this new strain so much more contagious than its predecessors. Researchers from the University of Arkansas say it all comes down to the stability of the infamous spike protein.
Graduate student Vivek Govind Kumar and the team from the lab of Mahmoud Moradi say the first step in any coronavirus infection is the virus entering a patient’s cells. To do this, the spike proteins on the surface of coronavirus cells (SARS-CoV) reposition to attack the body.
Over the years, scientists have learned what the “active” and “inactive” spike positions look like in both SARS-CoV-1 (the virus causing SARS) and SARS-CoV-2 (the virus causing COVID-19). Moradi’s group set out to uncover how these spikes switch from one position to another. To do this, they worked on molecular simulations at the Texas Advanced Computing Center and the Pittsburgh Supercomputing Center.
What makes COVID different from SARS?
Those simulations revealed that the coronavirus strain causing COVID-19 is incredibly more stable than even the SARS virus. Researchers explain that the main reason coronaviruses don’t usually spread rapidly is because their switches can’t stay on long enough to attack large populations.
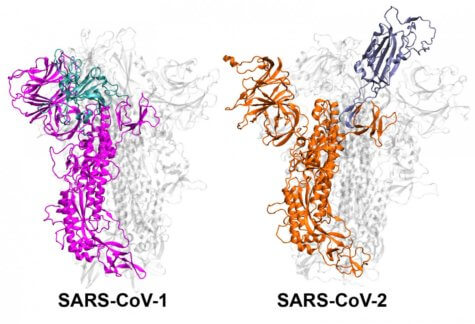
“We discovered in these simulations that SARS-CoV-1 and SARS-CoV-2 have completely different ways of changing their shape, and on different time scales,” Moradi says in a media release. “SARS-CoV-1 moves faster, it activates and deactivates, which doesn’t give it as much time to stick to the human cell because it’s not as stable. SARS-CoV-2, on the other hand, is stable and ready to attack.”
Moradi’s team also noted a region at the tail of SARS-CoV spike proteins scientists have generally ignored in past studies. The study finds that piece plays a key role in the stability of these spikes. Mutations in the tail could also impact the virus’s ability to infect people, the researchers warn. Learning more about how these switches work may also lead to a way of shutting down coronaviruses permanently.
“We could design therapeutics that alter the dynamics and make the inactive state more stable, thereby promoting the deactivation of SARS-CoV-2. That is a strategy that hasn’t yet been adopted,” Moradi explains.
Study authors add that the research may prove invaluable if a new coronavirus strain emerges in the future. Currently, the team is examining how switches in the new B.1.1.7 variant of the SARS-CoV-2 virus differ from prior mutations.
Researchers presented the findings at the 65th Annual Meeting of the Biophysical Society.