ERLANGEN, Germany — Many patients with COVID-19 can end up dealing with side-effects of their infection for weeks and even months after the illness clears. These “long hauler” cases of coronavirus have been something of a mystery to doctors. Now, however, a new study may have an answer as to why some people can’t seem to shake COVID-19. For the first time, researchers in Germany have discovered that the virus changes the size and stiffness of both red and white blood cells in the human body. Moreover, these changes can last for months, possibly explaining the seemingly never-ending symptoms of COVID-19.
A team from the Max Planck Center for Physics and Medicine used a technique called real-time deformability cytometry to examine thousands of blood cells from both COVID-19 patients and healthy individuals. Those tests reveal the size and deformability of red blood cells differs greatly between those contracting COVID and those who have not.
“We were able to detect clear and long-lasting changes in the cells — both during an acute infection and even afterwards,” reports Professor Jochen Guck, managing director of the Max Planck Institute for the Science of Light, in a media release.
‘Long COVID’ is a major problem
Researchers say some patients continue to struggle with shortness of breath, fatigue, and headaches long after a severe case of coronavirus. Sometimes, these side-effects persist for over six months. Previous studies have also discovered many recovering COVID patients also deal with neurological dysfunction and, in rare cases, problems with their heart.
One thing that has been clear about these infections is that COVID often impairs blood circulation. This can lead to dangerous blood clots and problems transporting oxygen throughout the body. All of these issues revolve around the blood cells and the importance of keeping them in proper shape.
Taking a picture of deformed blood cells
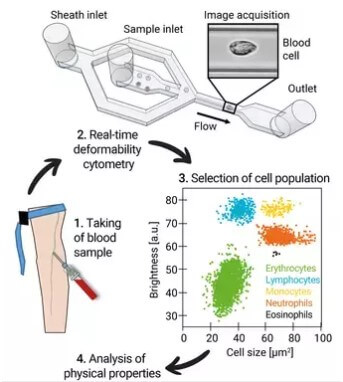
(© MPL/Guck Division)
Real-time deformability cytometry allowed the study authors to send blood cells through a narrow channel at high speeds. This process also stretches both the red and white blood cells which pass through, while a high-speed camera records each one with the aid of a microscope. When this is complete, custom computer software goes to work, determining how big and how deformed each cell is. Overall, RT-DC can analyze up to 1,000 blood cells per second.
In this study, researchers examined the blood of 17 patients with a severe case of COVID-19, 14 people who had recovered from a COVID infection, and 24 healthy volunteers. The drastic changes in the red blood cells between infected and uninfected individuals points to damage among COVID patients that could put them at increased risk for blockages and blood clots in their lungs. Additionally, results show the ability of a COVID patient’s red blood cells to carry oxygen appears to be impaired as well.
Study authors also discovered that lymphocytes (one type of white blood cell) are significantly softer in coronavirus patients. This typically happens when the body is having a strong immune reaction.
Another group of infection-fighting white blood cells, neutrophil granulocytes, appeared to change in the same way. The team notes these cells remained this way for several months after a patient’s infection.
“We suspect that the cytoskeleton of immune cells, which is largely responsible for cell function, has changed,” says study first author Markéta Kubánková.
Researchers believe this type of blood analysis could be key in future COVID-19 examinations as well as acting as an “early warning system” during future epidemics involving unknown viruses.
The study appears in the Biophysical Journal.