SHREVEPORT, La. — COVID-19 is typically associated with respiratory symptoms, but plenty of studies have shown how the disease can impact the brain. Research reveals that the SARS-CoV-2 virus can infiltrate neurons, leading to various neurological issues in COVID-19 patients. But how exactly does this happen?
Researchers say the susceptibility of neurons and astrocytes — specialized cells that safeguard neurons — to the SARS-CoV-2 virus may reveal why some individuals are more prone to develop neurological issues stemming from COVID-19.
“Our findings suggest that astrocytes are a pathway through which COVID-19 causes neurological damage,” says the study’s first author Ricardo Costa, Ph.D., a postdoctoral fellow at the Louisiana State University Health Shreveport, in a statement. “This could explain many of the neurologic symptoms we see in COVID-19 patients, which include loss of sense of smell and taste, disorientation, psychosis, and stroke.”
The SARS-CoV-2 virus makes its way into cells by binding to angiotensin-converting enzyme-2 (ACE2). This glycoprotein exists on the the surface of respiratory cells and was thought to be a common receptor throughout the body. However, scientists were unsure if it was present in brain cells.
The team investigated proteins and RNA segments to ascertain the existence of ACE2 glycoprotein on the surface of neurons and astrocytes. Finally, they inoculated the cells with a safer form of SARS-CoV-2.
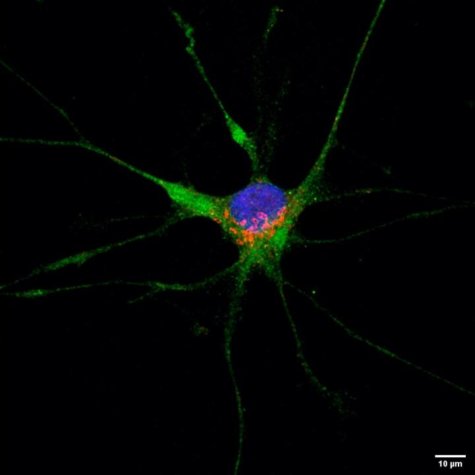
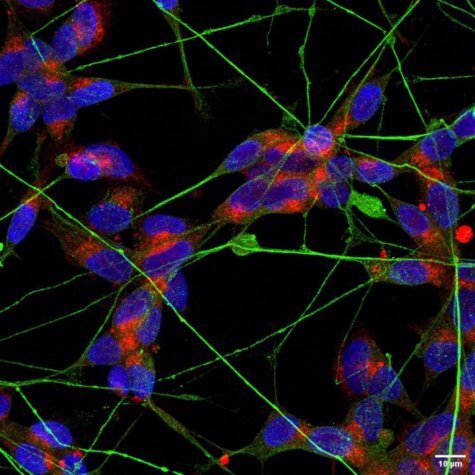
According to results, the COVID-19 virus is capable of infecting neurons and astrocytes. However, neurons were more prone to infection than astrocytes, according to the research.
Astrocytes form the blood-brain barrier that protects neurons from toxins in the bloodstream. They overlap each neuron and span the entire central nervous system, dropping off nutrients while preventing the flow of toxins. This means they are capable of guarding neurons from the COVID-19 virus. However, it also means they could be efficient at spreading the virus to a large number of cells if infected.
“While astrocytes display a higher resistance to infection, neurons seem to be more susceptible,” says Costa. “This suggests that only few astrocytes getting infected could be sufficient for the infection to quickly spread to neurons and multiply. These observations could explain why while some patients do not have any neurological symptoms, others seem to have severe ones.”
Costa discussed his findings at the American Physiological Society’s annual conference held electronically in April as part of the Experimental Biology 2021 event.