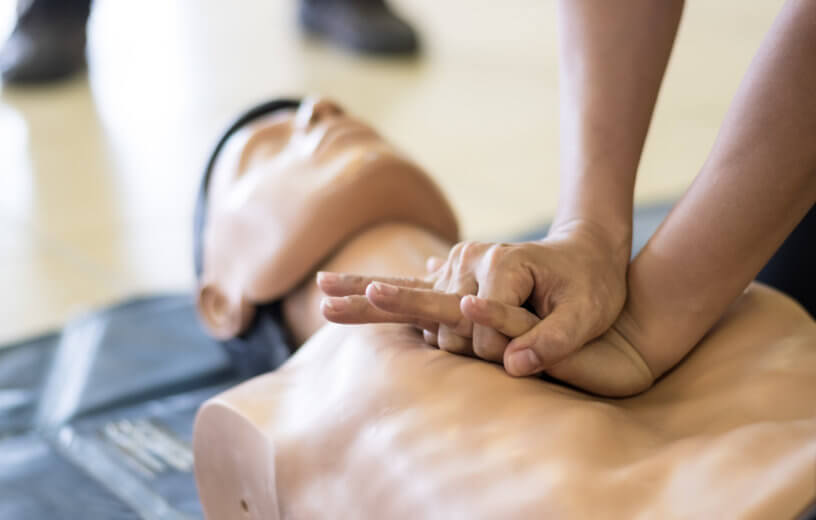
DENVER — While it may sound incredibly cruel and unfair, numerous studies have demonstrated that women are less likely than men to receive CPR in the event of an out-of-hospital cardiac arrest event. Now, new research has identified the main reasons behind this phenomenon: bystanders are concerned about the possibility of inappropriate contact or causing additional injury.
While the overall survival rate in the United States for cardiac arrest is less than 12%, CPR can double or even triple the sufferer’s odds of surviving.
The first study asked 54 online participants to explain why women may be less likely to receive CPR in public spaces. Aside from inappropriate touching concerns and fear of causing injury, other reasons that kept coming up in responses were: fear of being accused of sexual assault, poor recognition of a woman experiencing cardiac arrest, and the misconception that breasts hinder the effectiveness of CPR.
Male participants were far more likely to cite inappropriate touching concerns and fear of assault accusations than women. Meanwhile, more women mentioned a fear of causing more physical injury.
“The consequences of all of these major themes is that women will potentially receive no CPR or delays in initiation of CPR,” says study leader Dr. Sarah M. Perman, an assistant professor of Emergency Medicine at the University of Colorado School of Medicine, in a media release. “While these are actual fears the public holds, it is important to realize that CPR is lifesaving and should be rendered to collapsed individuals regardless of gender, race or ethnicity.”
While the study was too small and demographically narrow (60% male, and about 85% Caucasian) to form any definitive conclusions, Dr. Perman says the findings are nonetheless troubling. Especially the silly notion that CPR doesn’t work on women because of their breasts.
“Bystander CPR has been linked to better survival and neurologic recovery after out-of-hospital cardiac arrest. Quality chest compressions require that rescuers put their hands on the chest and push hard—regardless of (recipient’s) gender, the act of CPR is no different,” she adds.
A second study, performed in Philadelphia and led by Marion Leary, director of innovation research at the University of Pennsylvania’s Center for Resuscitation Science, used virtual reality to explore people’s responses to cardiac arrest events across genders. Virtual reality, the researchers say, was perfect for this topic because real-life cardiac emergencies happen quickly and leave little room for research.
All 75 of this study’s participants were not told what would happen in the virtual reality simulation, but were instructed to react just as they would in real-life. The virtual setting was a urban environment in which a pedestrian collapses while others cry out for help. Some participants were shown a male individual suffering a cardiac arrest, while others saw a female.
Participants performed CPR and helped male victims more often than female victims.
Regardless of the victim’s gender, “if you see someone collapse, call 911, begin CPR, and if there is an AED around, use it,” Leary says. “Doing something is better than doing nothing. You have the power to help save someone’s life.”
Both studies were presented at the American Heart Association’s Resuscitation Science Symposium in 2018.