NEW YORK — Americans are putting off essential medical appointments, and it’s not just because of the coronavirus pandemic, according to a new survey. But thanks to the rise of teleheath, more patients have grown comfortable with the idea of seeing a healthcare provider via video appointment.
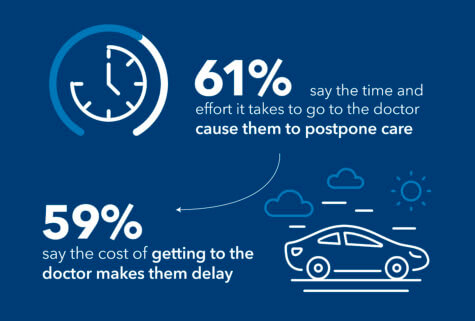
Seeing the doctor in the COVID era can be an unsettling experience for patients. So much so that many would simply rather not go at all. In fact, more than three out of four respondents say they have delayed everything from annual physicals and blood pressure checks to urgent care for an illness or injury. Sixty-one percent say that the time and effort it takes to visit a health care provider causes them to postpone getting the care they need. Another 59 percent say the cost of attending an in-person doctor’s appointment is what makes them delay.
Other reasons for postponing care include inconvenient appointment times (35%), the need to take time off work (29%), and the fear of being exposed to COVID-19 by other patients (17%). Delaying care has a cost of its own however, as 67 percent of respondents say they feel worried about their health when they put off a trip to the doctor.
Conducted by OnePoll on behalf of Kaiser Permanente, the survey of 2,000 Americans highlights how the use of telehealth, including video and telephone appointments, could help address the challenges many Americans face in getting to the doctor.
Why remote doctor appointments might be here to stay
Among the top benefits of telehealth identified by respondents, 54 percent say telehealth is convenient and 51 percent appreciate the travel time it saves them. The survey also revealed increased demand for telehealth in the wake of COVID-19.
 A staggering 98 percent of respondents report using telehealth with a provider since the pandemic began. This includes emailing a physician, dialing into a phone appointment, or having a video visit. Americans say face-to-face video visits are the most popular form of telehealth, with four in 10 using this option. Telephone appointments follow closely behind (39%).
A staggering 98 percent of respondents report using telehealth with a provider since the pandemic began. This includes emailing a physician, dialing into a phone appointment, or having a video visit. Americans say face-to-face video visits are the most popular form of telehealth, with four in 10 using this option. Telephone appointments follow closely behind (39%).
“The COVID-19 pandemic has sped the adoption of telehealth options that allow people to receive safe, high-quality care from the comfort of their homes,” says Arthur M. Southam, MD, executive vice president of Health Plan Operations for Kaiser Permanente, in a statement. “These ‘virtual house calls’ are appropriate for a wide range of health concerns and appointment types, ensuring there’s no reason to delay needed care.”
Increased use of telehealth may be a forgone conclusion, even after the COVID-19 crisis ends. Eighty-five percent of respondents say they’re likely to select telehealth for their next primary care appointment. Another 73 percent add they’re likely to choose it for their next specialty care appointment in areas such as dermatology or women’s health.
Perhaps the most telling sign that telehealth is here to stay is the more than 60 percent of respondents who report that the availability of telehealth is a factor – and in many cases a major one – in picking a health plan. Nearly eight in 10 think that telehealth should be universally available as a health care option within the next five years.
Bringing convenience to health care
 Convenience and integration are key factors in Americans’ willingness to consider telehealth. Nearly three in four people say they would be more likely to use telehealth if they knew their provider could order lab work, prescribe medications, and make referrals to other doctors using this technology.
Convenience and integration are key factors in Americans’ willingness to consider telehealth. Nearly three in four people say they would be more likely to use telehealth if they knew their provider could order lab work, prescribe medications, and make referrals to other doctors using this technology.
Four in five people cite the ability to follow up with their provider directly as being important to them in deciding whether to use telehealth. Seven in 10 said that they’d be more likely to choose telehealth if they knew a health care provider would have access to their full health history while using it.
“Today’s health care consumers expect and deserve to receive care in a way that’s flexible, convenient, and reflects their needs and preferences,” Dr. Southam says. “It’s the health care industry’s obligation to meet those expectations by providing a fully integrated experience — one that enhances patients’ experiences, improves their health outcomes, and expands their access to high-quality care.”
